ADHD and bipolar depression are two distinct conditions that frequently get mixed up, even by people seeking care. Many patients experience symptoms that overlap, making it genuinely difficult to tell them apart without expert evaluation.
At Alice’s Psychiatry and Wellness, we’ve seen firsthand how misdiagnosis delays proper treatment. Getting the right diagnosis matters because the medications and strategies that work for one condition can actually worsen the other.
What Sets ADHD and Bipolar Depression Apart
ADHD is a neurodevelopmental condition that starts in childhood and affects how the brain processes attention, impulse control, and executive function. The core problem is persistent symptoms of inattention, hyperactivity, and impulsivity. These challenges don’t come and go-they’re stable across situations and throughout life. A person with ADHD struggles to finish work projects, loses track of time, interrupts conversations frequently, or acts without thinking through consequences. The symptoms often appear less noticeable in adulthood than childhood because people develop workarounds, but the underlying attention and impulse control difficulties remain.
Bipolar depression is fundamentally different. It’s a mood disorder characterized by episodes-distinct periods where mood shifts dramatically and lasts for days or weeks. During a depressive episode, a person experiences persistent sadness or irritability, loss of interest in activities, appetite or sleep changes, low energy, poor concentration, and sometimes suicidal thoughts. The key distinction is that bipolar depression is episodic, not constant. A person might feel fine for months, then slip into a depressive episode. Bipolar disorder also includes manic or hypomanic episodes where mood becomes abnormally elevated, energy surges, judgment becomes impaired, and risky behavior increases. Many people wait years for an accurate diagnosis because the condition gets misidentified as unipolar depression or ADHD.
The Symptom Overlap Problem
Impulsivity, distractibility, and irritability appear in both conditions, which is where the confusion starts. Someone in a manic episode might seem hyperactive and scattered like ADHD. Someone with ADHD might seem moody and irritable. But the timing and triggers differ sharply. ADHD impulsivity is persistent-it happens whether someone is happy, sad, or neutral. Bipolar impulsivity occurs primarily during mood episodes and reflects poor judgment driven by elevated or depressed mood.
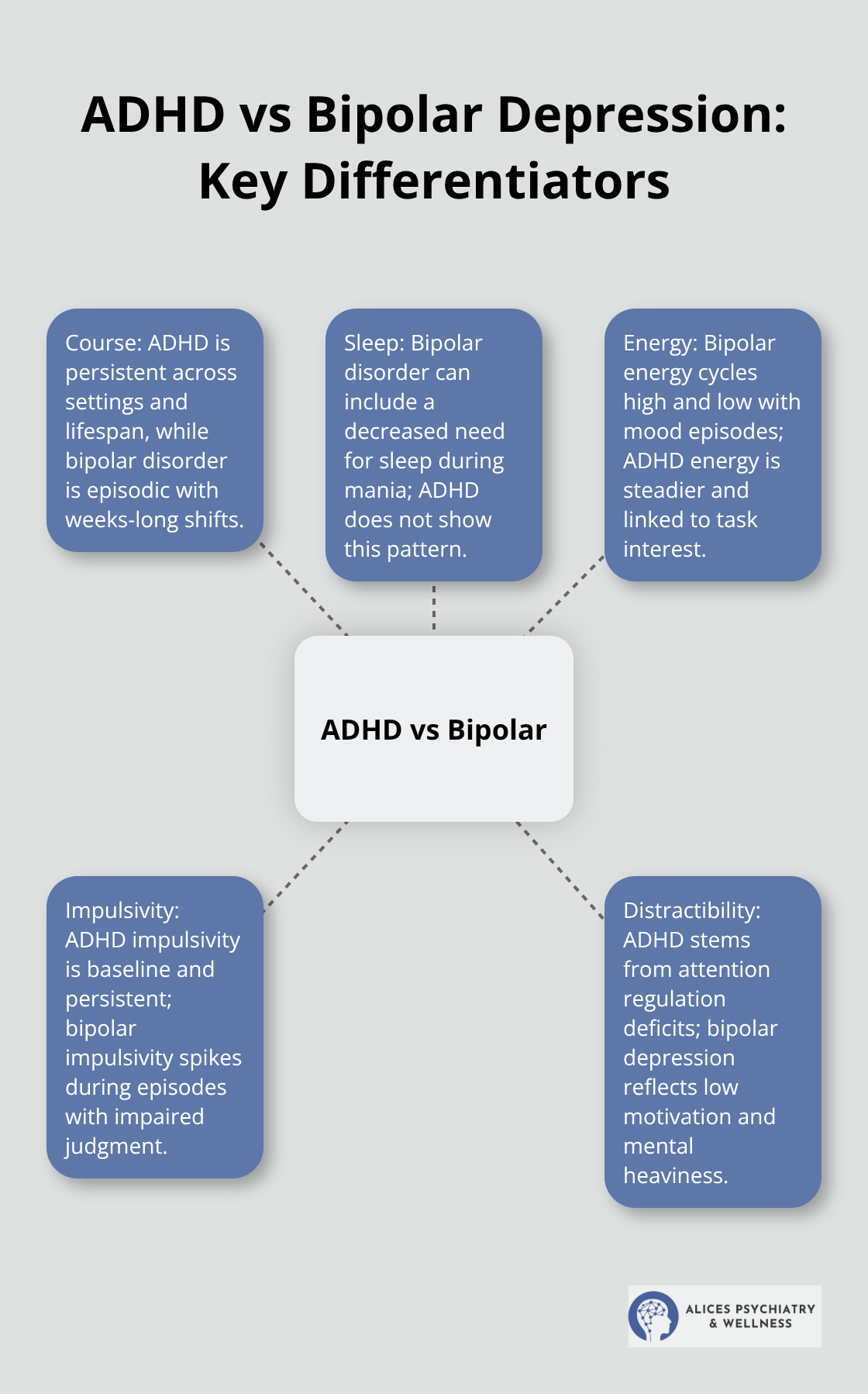
ADHD distractibility stems from attention regulation problems; bipolar distractibility during depression comes from low motivation and mental heaviness. A person with ADHD struggles to organize a project from start to finish. A person in bipolar depression struggles to care about the project at all.
Sleep and Energy Patterns Reveal the Difference
Bipolar patients often report a decreased need for sleep during manic or hypomanic episodes-they feel rested after just a few hours. ADHD doesn’t involve this pattern. Sleep problems in ADHD tend to be variable and less distinctive. Bipolar patients also experience cyclical energy changes tied to mood episodes: intense energy during mania, profound fatigue during depression. ADHD energy tends to be more constant and tied to external stimulation or task interest. When a bipolar patient enters a depressive episode, that low energy is internal and persistent. When someone with ADHD loses focus on a boring task, they perk up immediately with something engaging.
How Mood Episodes Distinguish Bipolar Depression
Bipolar depression arrives in waves. A person might wake up one morning and feel the weight of depression settle in-sadness, emptiness, or irritability that persists for weeks regardless of what happens around them. This internal shift is the hallmark of bipolar disorder. ADHD doesn’t work this way. Someone with ADHD experiences mood fluctuations tied to external events or task difficulty. They feel frustrated when a project feels overwhelming, then shift quickly once the task changes. The bipolar depressive episode, by contrast, colors everything. A person in bipolar depression finds little pleasure in activities they normally enjoy, experiences appetite changes, and struggles with concentration that feels different from ADHD attention problems-it’s driven by low motivation and mental fog rather than impulse control issues. The episode eventually lifts, sometimes naturally, sometimes with treatment, but the cyclical nature of bipolar mood episodes is what separates this condition from ADHD’s more stable, persistent presentation.
Understanding these differences matters because treatment approaches diverge significantly. Recognizing whether someone’s struggles stem from attention regulation problems or episodic mood shifts changes everything about how we approach care. If you’re navigating these questions in Lilburn, GA or Atlanta, GA, our team at Alice’s Psychiatry and Wellness is here to help clarify your symptoms and guide you toward the right support. This distinction becomes even more important when both conditions exist together-a reality that affects many people seeking help.
When ADHD and Bipolar Disorder Exist Together
The overlap between ADHD and bipolar disorder is far more common than many people realize. Research shows that approximately 10 to 20 percent of adults with bipolar disorder also meet criteria for ADHD, while roughly 15 to 25 percent of adults diagnosed with ADHD may develop bipolar disorder over their lifetime. This co-occurrence isn’t coincidental-it reflects genuine biological overlap.
The Severity of Comorbidity
When both conditions exist together, the clinical picture becomes significantly more severe. Studies from the Archives of General Psychiatry and the Journal of the American Academy of Child and Adolescent Psychiatry document that patients with comorbid ADHD and bipolar disorder experience earlier mood episode onset, shorter periods of stability between episodes, more frequent cycling, and greater irritability and aggression compared to those with bipolar disorder alone. The genetic research is particularly revealing: scientists have identified approximately 30 shared risk loci between ADHD and bipolar disorder, indicating a substantial shared biological vulnerability.
Shared Risk Factors Across Generations
Environmental factors increase risk for both conditions alongside genetic predisposition. Maternal substance use during pregnancy, maternal stress, and adverse childhood experiences all elevate the likelihood of developing either or both conditions. This genetic and environmental overlap explains why some families show multiple members affected by these conditions across generations.

Why Medication Sequencing Matters
The practical challenge this creates is substantial: stimulant medications prescribed for ADHD can trigger or worsen manic episodes in people with bipolar disorder, making standard ADHD treatment potentially dangerous without proper mood stabilization first. Treatment sequencing matters tremendously. The evidence-based approach starts with stabilizing mood through mood stabilizers or other bipolar-specific medications before attempting to address ADHD symptoms. Once bipolar symptoms are controlled, ADHD medications can be introduced with careful monitoring, or non-stimulant alternatives like atomoxetine may be considered.

Starting therapy while beginning medication means you attack the problem from multiple angles simultaneously.
Diagnostic Accuracy Requires Structured Assessment
A structured diagnostic process is essential-specialists should use formal ADHD interviews rather than brief screening tools. The timing of symptom onset provides vital diagnostic information: ADHD symptoms must have appeared before age 12, while bipolar mood episodes typically emerge later, often in late adolescence or early adulthood. If you experience persistent attention struggles alongside episodic mood shifts, seeking evaluation from a clinician experienced in both conditions is vital. The distinction between these conditions shapes everything about your treatment plan, from which medications you receive to how your care unfolds over time.
How to Treat ADHD and Bipolar Depression Together
Treating comorbid ADHD and bipolar disorder requires a deliberate, sequenced approach that prioritizes mood stabilization first. This isn’t a compromise or theoretical best practice-it’s essential because stimulants used for ADHD can trigger or intensify manic episodes in people with bipolar disorder. The evidence is clear: mood stabilization must be the foundation.
Establishing Mood Stability as the Treatment Foundation
Once a person’s bipolar symptoms are controlled through medications like lithium, valproate, or lamotrigine, ADHD symptoms often improve somewhat on their own because better mood regulation enhances focus and impulse control. Research from the Journal of Clinical Psychiatry shows that bipolar patients with comorbid ADHD experience nearly three times more instability over a two-year period when treatment doesn’t address both conditions systematically. This means the stakes are high for getting the order right. Clinicians start every comorbid case by establishing mood stability first, then wait four to six weeks to assess whether ADHD symptoms persist after mood episodes resolve. Many patients report meaningful improvement in attention and impulse control once their mood stabilizes, which can reduce or eliminate the need for ADHD medications entirely.
Choosing the Right ADHD Medications After Mood Stabilization
When ADHD symptoms do remain after mood stabilization, non-stimulant options like atomoxetine or guanfacine become the first choice because they carry lower risk of mood destabilization compared to amphetamines or methylphenidate. If a stimulant becomes necessary, clinicians introduce it at a low dose with close monitoring-typically weekly check-ins for the first month to catch any mood shifts early. This cautious approach protects against the risk that stimulants pose to people with bipolar disorder while still addressing persistent attention and impulse control problems.
Therapy and Behavioral Strategies Work Alongside Medication
Cognitive behavioral therapy helps people recognize the specific triggers and patterns of their ADHD symptoms, while also teaching mood monitoring skills essential for bipolar management. Psychoeducation about the two conditions separately and together prevents the confusion that often delays treatment adherence. Many people stop taking medications because they don’t understand why a mood stabilizer matters when their main complaint is attention problems, or why a stimulant feels risky when their energy is already scattered. Practical behavioral strategies include structured sleep schedules, which matter more for bipolar disorder than ADHD alone because sleep disruption is a known trigger for mood episodes, and external organizational systems like calendars and task management apps that compensate for ADHD-related executive function gaps without requiring medication adjustments.
Lifestyle Interventions That Support Both Conditions
Regular exercise reduces both ADHD restlessness and bipolar mood cycling-research consistently shows that 30 minutes of aerobic activity most days improves outcomes for both conditions. Sleep consistency, stress management, and social connection all stabilize mood while reducing ADHD-related impulsivity and attention problems. These lifestyle factors work best when combined with medication and therapy rather than as standalone treatments. If you’re in Lilburn, GA or Atlanta, GA and managing these overlapping challenges, accurate diagnosis from a specialist experienced in both ADHD and bipolar disorder is non-negotiable. The difference between a clinician who screens for both conditions and one who treats them separately often determines whether treatment succeeds or fails.
Final Thoughts
Accurate diagnosis determines whether your treatment succeeds or fails when you have ADHD and bipolar depression. If you experience persistent attention struggles, impulsivity, or hyperactivity alongside episodic mood shifts, you need evaluation from a clinician experienced in recognizing both conditions. Many people spend years receiving incomplete or incorrect treatment because one condition gets identified while the other remains hidden, and the overlap in symptoms makes this confusion understandable, but the consequences are serious.
Seek professional help if you notice mood episodes lasting weeks, decreased need for sleep during high-energy periods, or persistent attention and impulse control problems that started in childhood. If you have a family history of bipolar disorder or ADHD, that increases the importance of comprehensive evaluation. If your current treatment isn’t working or you suspect you might have both conditions, don’t wait-the longer comorbid ADHD and bipolar depression go unrecognized, the more severe the clinical course becomes.
We at Alice’s Psychiatry and Wellness specialize in comprehensive psychiatric evaluations that assess for both conditions simultaneously through detailed history-taking and structured assessment. Whether you’re in Lilburn, GA, Atlanta, GA, or accessing care through our telepsychiatry services, our team is equipped to provide the accurate diagnosis and coordinated treatment that makes the difference. Your mental health deserves expertise and care that addresses your complete clinical picture, not just isolated symptoms.








