Psychiatric medications work differently for every person, and understanding how they function is the first step toward finding what works for you. We at Alice’s Psychiatry and Wellness know that psychiatry pharmacology can feel overwhelming, especially when you’re navigating treatment options for the first time.
This guide breaks down medication classes, personalized approaches, and real answers to your concerns-so you can make informed decisions with your provider.
What Psychiatric Medications Actually Do
How Antidepressants Target Brain Chemistry
Psychiatric medications work by targeting specific brain chemicals to reduce symptoms and improve your quality of life. They’re not a cure, but they’re a cornerstone of effective treatment. Antidepressants like selective serotonin reuptake inhibitors (SSRIs) block your brain from reabsorbing serotonin-a neurotransmitter that regulates mood, sleep, and memory. This action means more serotonin stays available in your brain, which helps lift depression and anxiety. SSRIs rank as the most frequently prescribed antidepressants because they’re effective and tend to have fewer side effects than older options. If you have depression or anxiety, your provider will likely consider an SSRI first, with sertraline and escitalopram among the most commonly used choices.
Antipsychotics for Severe Conditions
Antipsychotics work through a different mechanism-they block dopamine receptors to reduce symptoms like hallucinations and delusions. Newer antipsychotics, called atypical antipsychotics, are preferred over older versions because they carry a lower risk of movement-related side effects. Your provider may prescribe them for schizophrenia, bipolar disorder, or sometimes severe depression that hasn’t responded to other treatments.
Anti-Anxiety Medications and Mood Stabilizers
Anti-anxiety medications and mood stabilizers serve distinct purposes in mental health treatment. Benzodiazepines like alprazolam provide fast relief for acute anxiety or panic, but they carry real risks of dependency with long-term use-which is why doctors typically reserve them for short-term situations. For ongoing anxiety management, many providers prescribe antidepressants or buspiron instead, which work more gently without the addiction potential. Mood stabilizers like lithium and valproate help manage bipolar disorder by reducing the intensity of manic and depressive swings. Lithium stands out as particularly effective, but it requires regular blood tests every 3 to 6 months to keep levels safe, and it affects your kidneys and thyroid over time.
Your Unique Response to Medication
Understanding how these medications work gives you the foundation to have meaningful conversations with your provider about what might work for your specific situation. Your genetics, other medications, lifestyle, and medical history all influence which medication will actually help you. Treatment works best when medication combines with therapy, whether that’s cognitive behavioral therapy or psychotherapy. This dual approach addresses both the biological and psychological aspects of mental health, leading to stronger, longer-lasting improvement.
Your provider will work with you to identify the right fit-and that process often involves pharmacogenetic testing to understand how your unique genetic makeup affects medication response. This scientific approach helps skip the guesswork and gets you on the right treatment faster. With this foundation in place, the next step involves learning how personalized medication management and genetic testing can transform your treatment plan.

Personalized Medication Management and Pharmacogenetics
Pharmacogenetic testing removes the trial-and-error approach from medication selection. Instead of starting an antidepressant and waiting weeks to see if it helps, your provider can analyze how your genes affect medication metabolism and response. The test examines cytochrome P450 enzymes-the proteins your body uses to break down psychiatric medications.

If you metabolize medications slowly, a standard dose may accumulate to toxic levels; if you metabolize quickly, you might need higher doses to feel any benefit. Knowing this upfront means your provider prescribes the right dose on day one, not after months of adjustments. Studies show that pharmacogenetic-guided treatment leads to faster symptom improvement and higher remission rates compared to standard prescribing.
How Genetic Testing Guides Treatment Plans
Your genetic profile reveals which medications your body tolerates well. Some people carry variants that increase the risk of specific side effects, and testing identifies these before they become problems. For example, certain genetic markers predict whether you’ll experience weight gain from antipsychotics or sexual dysfunction from SSRIs. Your provider uses this information to select medications that align with your health priorities and lifestyle. If weight management matters to you, your provider might choose an antipsychotic with a lower metabolic burden. If sexual side effects are a dealbreaker, testing helps identify antidepressants you’re more likely to tolerate. This personalized approach isn’t just about comfort-it’s about adherence. When patients experience fewer side effects, they stay on medications longer and see better outcomes.
Minimizing Side Effects Through Personalized Approach
Genetic data transforms how your provider selects medications by predicting your individual response before treatment starts. Rather than discussing theoretical medication options, you’re discussing choices backed by your biology. This scientific foundation means your provider avoids medications that carry high risks for you specifically. If you work long hours and fatigue already drains your energy, your provider can avoid medications that worsen drowsiness. If you’re planning to get pregnant, your provider needs to know so medication safety during pregnancy guides the choice. Past medication experiences matter too-if you’ve tried an antidepressant before and it didn’t work, pharmacogenetic testing may reveal why (perhaps you metabolize it too quickly, or your genes predict poor response).
Working with Your Provider to Find the Right Medication
The conversation between you and your provider transforms once genetic data enters the picture. Bring your concerns about side effects, your lifestyle constraints, and your treatment goals to this conversation. Talk openly about what matters most to you-whether that’s maintaining your energy, protecting your sexual function, or avoiding weight changes. Your provider uses all this information alongside genetic results to build a plan that actually fits your life. This collaborative approach means you’re not passive in treatment; you’re an active partner shaping decisions. Your provider listens to your priorities and combines them with pharmacogenetic insights to identify medications that work with your body, not against it. With your personalized medication plan in place, the next step involves addressing the concerns and questions that often arise as you begin treatment.
What Should You Actually Expect From Psychiatric Medications
Understanding Initial Side Effects and Timeline
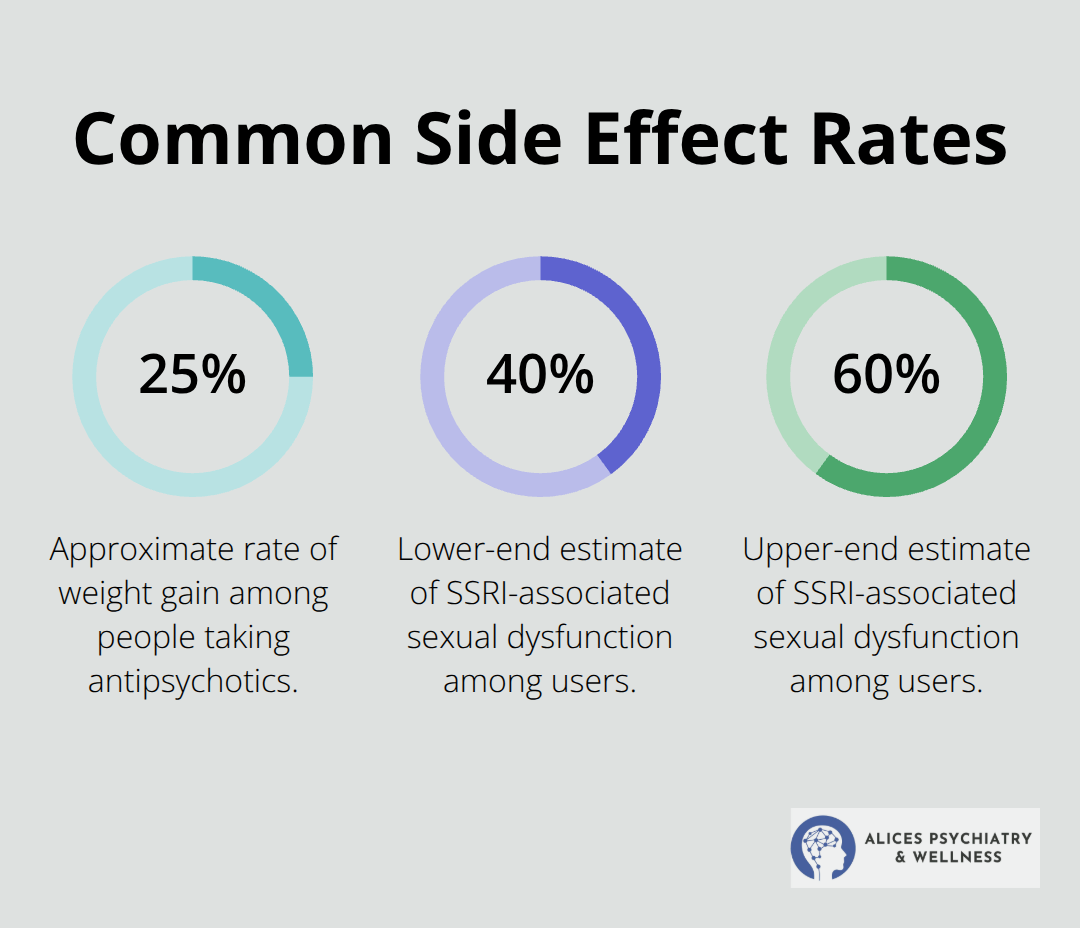
Side effects are real, but they’re not inevitable, and they’re not permanent. When you start a psychiatric medication, your body needs time to adjust-typically 4 to 6 weeks before you notice meaningful symptom relief. During those first weeks, you might experience temporary side effects like nausea, headaches, drowsiness, or changes in appetite. These initial reactions often fade as your body adapts, but some side effects persist. Weight gain affects roughly 25 percent of people taking antipsychotics, while SSRIs can cause sexual dysfunction in 40 to 60 percent of users. These aren’t small concerns, and your provider should address them directly rather than dismissing them as minor.
Taking Action When Side Effects Occur
If a side effect significantly impacts your quality of life, tell your provider immediately-don’t wait for your next scheduled appointment. Your provider can adjust your dose, switch to a different medication, or add another medication to counteract the side effect. For example, if an SSRI causes sexual dysfunction, adding bupropion often restores sexual function without stopping your antidepressant. If weight gain becomes problematic, your provider might switch you to an antipsychotic with a lower metabolic burden or recommend lifestyle adjustments that actually work. The key is honest communication; your provider can’t help solve problems they don’t know exist.
Benzodiazepines and Dependency Risks
Dependency concerns stop many people from taking benzodiazepines, and that caution is justified for long-term use. Benzodiazepines work quickly for acute anxiety or panic, but using them daily for more than 3 to 4 weeks increases your risk of physical dependence. This doesn’t mean you’re weak or addicted-it means your brain adapts to the medication’s presence, and stopping abruptly causes withdrawal symptoms like rebound anxiety, insomnia, and tremors. If you’ve taken benzodiazepines regularly for months, your provider needs to taper your dose gradually over weeks or months rather than stopping cold turkey. Other psychiatric medications like SSRIs and antipsychotics don’t create the same dependency risk, though stopping them suddenly can cause discontinuation symptoms.
Combining Therapy With Medication for Maximum Impact
Therapy transforms medication’s effectiveness in ways medication alone cannot achieve. Research consistently shows that combining antidepressants with cognitive behavioral therapy produces better outcomes than either treatment alone. Therapy teaches you skills to manage negative thought patterns, process trauma, and build resilience-changes that stick with you long-term. If you’re in Lilburn, GA or Atlanta, GA and seeking integrated care that combines medication management with therapy, we at Alice’s Psychiatry and Wellness coordinate both approaches to maximize your progress. Medication addresses the biological side of mental health, but therapy addresses the behavioral and psychological patterns that keep symptoms alive. Starting therapy while beginning medication means you attack the problem from multiple angles simultaneously, which accelerates improvement and reduces relapse risk.
Final Thoughts
Psychiatric pharmacology works best when you treat medication as one tool within a larger strategy that includes therapy, lifestyle changes, and honest conversations with your provider. Your genetics matter, your side effects matter, and your preferences matter-a provider who listens to all three and combines that insight with scientific evidence gives you the best chance at real improvement. This partnership between you and your provider transforms treatment from guesswork into precision care.
Finding the right medication takes time and patience, and your first choice might not be your final choice. What matters is that you stay engaged in the process, communicate openly about what’s working and what isn’t, and trust that adjustments will happen. If you’re in Lilburn, GA or Atlanta, GA and ready to start this journey with a provider who specializes in personalized medication management, Alice’s Psychiatry and Wellness is here to support you.
Your mental health deserves expert, compassionate care that treats you as a whole person, not just a diagnosis. Take that first step today.








